Jaw (TMJ) pain is a common problem that can be treated by a physiotherapist. Luke, a physiotherapist from our Burnside practice outlines what the TMJ is, as well as the symptoms and treatment of TMJ disorders.
What is The TMJ?
The TMJ is located at the area where our mandible (jaw) meets the temporal bone of our skull. Both of these structures are characterized by fibrocartilaginous surfaces with an articular disc in between the temporal bone and mandible, which separates the joint into an upper and lower compartment.
You can find your own TMJ by placing a finger at the front of your ear on either side, then searching ~1-2cm forward and pressing with a somewhat firm push into your jaw. Then, open and close the mouth and you should feel a prominent bony structure moving up and down. This is your head of the mandible (jaw) which inserts into the temporal bone of your skull.
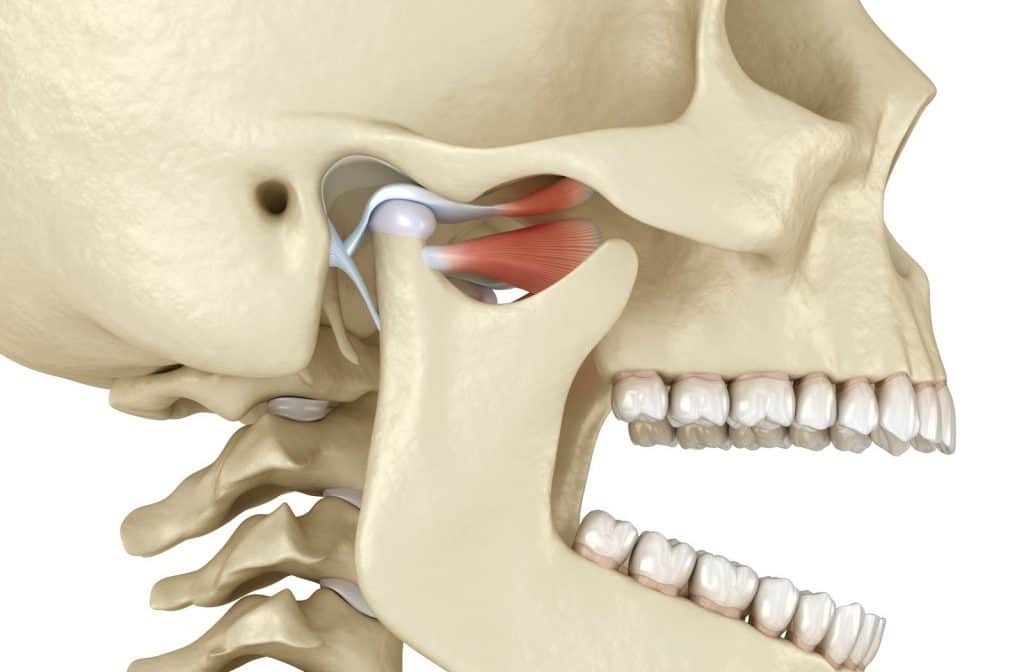
The core anatomical function of the mandible (jaw) is to open (depress), close (elevate), protrusion (push jaw forward), retrusion (pull jaw back) and lateral deviation (move side to side). There are a range of muscles that act on the mandible to complete these movements.
These muscles play an important role in the function of breathing, eating and swallowing. These muscles also contribute to bruxing, which is grinding the teeth with and / or without contact of top/bottom teeth. Bruxing is common during sleep and in times of increased stress. Both factors can lead to increased prevalence of TMJ dysfunction and disorders.
Symptoms of TMJ Disorders
TMJ disorders often present with aching or pain around the neck, cheeks, temples, ears, teeth or jaw. Common reported symptoms of TMJ disorders include:
- Lateral (side) or posterior (back) headaches or aching
- Tinnitus (ringing in the ears)
- Pain with eating, singing, talking, yawning or chewing
- Jaw clicking, locking or grinding
- Pain/tenderness of the jaw
- Deviation of the jaw to one side when opening/closing

These symptoms can arise from a variety of causes, such as a history of grinding or clenching teeth during sleep, arthritis (osteoarthritis, rheumatoid arthritis), jaw injury, dentistry procedures (jaw remodelling, tooth extraction) and emotionally or physically stressful events. It is also important to rule out your cervical spine (neck) as a source of symptoms, as cervical dysfunction can refer pain in the area of your TMJ. Symptoms in the cervical spine may stem from, but are not limited to trauma, poor postures or biomechanical dysfunction.
Treatment
A physiotherapist will start by assessing your jaw range of movement, muscle strength, muscle length, motor control and movement patterns. This can help determine if your symptoms are related to one of the following:
- TMJ (Joint) disorder
- Cervical spine pathology
- Muscle disorder
- Developmental
- Locked open joint disorder (intermittent or permanent)
- Jaw occlusion
- Arthritic
- Inflammatory / inflammation
- Dislocation or derangement of disc/condyle
The primary treatment of TMJ dysfunction is to reduce pain, increase oral motor function with activities such as chewing or talking and improve joint mobility/health.
Physiotherapy techniques to treat TMJ dysfunction may include manual therapy (either through external means or internal techniques) to reduce pain and increase range of movement, joint mobilisation techniques, muscle stretching exercises (passive and active), dry needling, postural exercises and muscle strengthening exercises.
Additional options for conservative TMJ dysfunction treatment may include postural changes, changing types of foods consumed, medication, jaw relaxation techniques or thermal modalities (heat/wheat packs).
This blog was written by Luke Mrowka (Physiotherapist), from our Burnside practice.
References
Aggarwal, A. and Keluskar, V., 2012. Physiotherapy as an adjuvant therapy for treatment of TMJ disorders. General dentistry, 60(2), pp.e119-22.
Karthikeyan, P. and Kumaresan, R., Temporomandibular disorders & physiotherapy-a review. Turkish Journal of Physiotherapy and Rehabilitation, 32, p.3.
Fale, H., Hnamte, L., Deolia, S., Pasad, S., Kohale, S. and Sen, S., 2018. Association between parafunctional habit and sign and symptoms of temporomandibular dysfunction. Journal of Dental Research and Review, 5(1), p.17.

